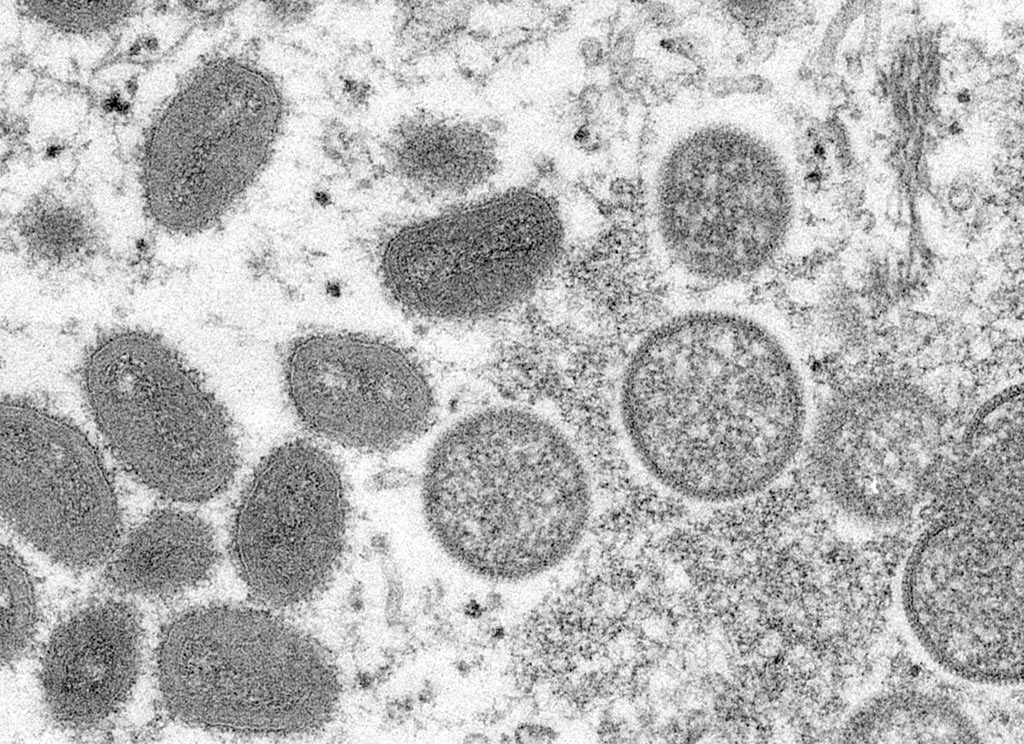
Cases of monkeypox in America have increased 46% in the last week, reported the Pan American Health Organization (PAHO), which has confirmed 1,325 cases in the region, representing 15% worldwide. Most infections have occurred in men over the age of 30 and in people from the LGBTQ+ community.
Of the total number of confirmed cases, 81% were reported from the United States of America and Canada, where the number of cases rose sharply following the return to mass gatheringssomething that was also observed in Brazil and Peru”, explained the Director of PAHO, Carissa F. Etienne.
According to the PAHO report, so far the most affected groups are men between 30 and 49 years. Likewise, the official emphasized that prevention and early detection actions should be focused on the highest risk groups such as people of sexual diversity.
“It is important to mention that in many countries in the region, where we have well-characterized information, the proportion of cases with no travel history is increasing every epidemiological week, which highlights our concern in establishing a more sustained transmission,” added Jairo Méndez Rico, PAHO adviser on emerging viral diseases, at a press conference.
In America, cases of monkeypox have been identified in the United States, Canada, Brazil, Mexico, Peru, Chile, Argentina, Colombia, the Bahamas, Ecuador, Jamaica, Panama, the Dominican Republic, and Venezuela. 81% of infections have been reported in North America, but in recent weeks there has been an increase in Brazil and Peru.
According to the “Epidemiological Update on monkeypox” report, published on July 9, 2022, Among the confirmed cases there are 113 health workers, but it is being investigated whether the infection in these was caused by exposure to the disease. Likewise, it details that of the total cases reported in America, 9% required hospitalization for isolation or treatment and there were two that were taken to the Intensive Care Unit (ICU).
“The true magnitude of the outbreak is likely to be underestimated in countries that have not previously reported monkeypox cases due to late clinical diagnosis and lack of access to laboratory tests. There is the possibility of a greater impact of the outbreak due to the affectation of vulnerable groups”, says PAHO.
Monkeypox in the LGBTQ+ population
PAHO marks an inclination to spread cases in the LGBTQ+ population. Officials assure that, of the cases with available information by gender, 98% were identified as men who have sex with men (MSM), and of these, 41% are HIV positive, detailed in their epidemiological update report.
PAHO’s Deputy Director of Health Emergencies, Sylvain Aldighieri, stresses that the increase in smallpox cases would be related to two facts: the holding of massive events for LGBTQ+ Pride month and the expansion of epidemiological surveillance to find more cases.
“I believe that if there is a factor that explains the increase in the number of cases in this region at this time: they are the multiple massive events that were organized in the month of June, within the framework of the ‘Pride Month’. That’s because our organization’s focus on advising countries and community groups to alert and ensure prevention in high-risk groups such as “LCM”men who have sex with men”, said Dr. Aldighieri, at a press conference.
Since last May, the UN Program dedicated to HIV/AIDS, UNAIDS, expressed its concern about the stigma that is growing towards LGTBI and African people by linking this disease to these groups that have historically suffered discrimination and racism.
The UN warned that this could undermine efforts to stop the outbreak, as a “climate of fear” will keep many people from seeking health services.
Monkeypox is not a sexually transmitted disease, nor is it exclusive to a specific group. all people are exposed. Infection occurs through contact with wounds, body fluids, droplets and contaminated material, and its incubation period is usually six to thirteen days, although it can be up to three weeks.
Likewise, Aldighieri explains that the increase in cases is also related to the greater detection capacity, “When there are no laboratories, there are no confirmed cases. When there are laboratories accessible to the health network, including the private sector, there are more case notifications”.