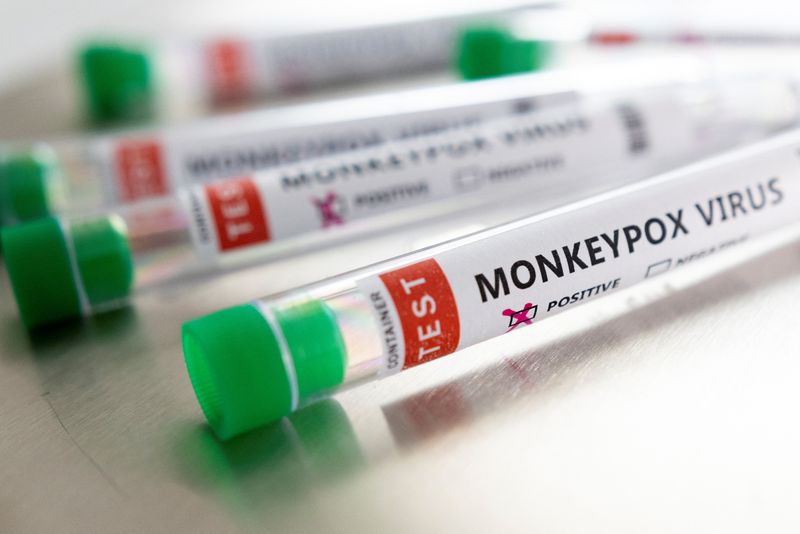
From the end of April onwards, 18,894 cases of monkeypox have already been reported and the world today faces another public health emergency of international importance, just like COVID-19. The majority of affected patients are men who have sex with other men, although some cases have also been reported in women and children.
Although the causes of this outbreak that affects people in more than 70 countries are being investigated, today the question arises:
Is the world facing a new sexually transmitted infection like HIV or syphilis?
During today’s session it was learned that for the first time two people died in places that had not yet detected deaths. These are Brazil and Spain The Spanish Ministry of Health reported this Friday the first death from monkeypox in that country and confirmed that there were 4,298 cases of infected people in its territory, according to the latest report from the National Epidemiological Surveillance Network ( Renave),
Brazil, meanwhile, also reported today its first death related to monkeypox, according to a statement from the Ministry of Health confirming the death of a 41-year-old man who suffered from cancer and had a weakened immune system.
Monkeypox was given that name in 1958 when it was detected in several laboratory apes in Denmark. In 1970 the virus was detected in humans. It is considered a zoonotic viral disease, which means it can be transmitted from animals to humans. It can also be transmitted from human to human. It is known that the disease is transmitted by direct contact with the lesions of an infected patient or by surfaces contaminated by them, but little is known about the possible presence of viruses in other biological samples, such as saliva, urine or semen.
In Spain, a study was carried out that was published in the journal Eurosurveillance, and contributes to a better understanding of how this emerging disease is transmitted. Viral DNA can frequently be detected in different clinical samples from patients infected with monkeypox, including saliva and semen, according to the work led by the Barcelona Institute for Global Health (ISGlobal), a center promoted by the “la Caixa” Foundation. ”.
Most of those affected so far are men. However, the disease has spread to many other countries and there is concern that it may spread to vulnerable population groups, such as immunocompromised patients or children.
In this study, the team led by Mikel Martínez, an ISGlobal researcher, and José Luis Blanco, from the Hospital Clínic de Barcelona, investigated the presence of genetic material from the virus in different biological samples, collected at different times, from 12 patients with confirmed infection for monkeypox. At the time of diagnosis, a high viral DNA load was detected in the skin lesions of all patients.
Furthermore, DNA was detected in the saliva of all patients, some of them with high viral loads. Only one previous study had tested saliva, in a single patient. Viral DNA was also detected in 92% of rectal samples, 83% of nasopharyngeal samples, 78% of semen samples, 75% of urine samples, and 67% of fecal samples.
“A couple of previous studies had already shown the occasional presence of viral DNA in some samples and in some patients, but in this study we show the frequent presence of viral DNA in various biological fluids, particularly in saliva, during the acute phase of the disease, and up to 16 days after the onset of symptoms in one patient,” explained Aida Peiró, ISGlobal researcher and first author of the study.
The authors point out that the presence of viral DNA does not necessarily equate to the presence of infectious virus, and that the next step will be to try to isolate infectious virus from these samples. However, the high viral load detected in saliva or semen suggests that these fluids have infectious potential, they add. “The results of our study contribute to a better understanding of the mechanisms and dynamics of virus transmission, as well as the possible role of sexual transmission,” said Martínez.
Consulted by Infobae, Dr. Gustavo Lopardo, vice president of the Pan American Association of Infectious Diseases and teaching coordinator of FUNCEI in Buenos Aires, explained: “Spekepox is a disease that is transmitted by very close contact, and that is currently behaving like a sexually transmitted infection. Most of the people who have been diagnosed are men who have relationships with other men.”
The expert Lopardo clarified: “The virus can be detected in semen, but it is very likely that it is being transmitted through skin contact with lesions of the person with the infection. We are observing that most of the lesions are occurring in the genital region of the affected people. This is a big difference from the cases that have been reported in Africa. Another difference is that most patients have mild symptoms”.
Meanwhile, the coordinator of the monkeypox working group of the Spanish Society of Infectious Diseases and Clinical Microbiology (SEIMC), Javier Membrillo, stated that, from the clinical side, “one thing is that a positive test is found in semen, and another thing is that this virus is transmitted. In fact, saving the distance, he recalls the case of people with a positive PCR for COVID-19 but who are not contagious. That monkeypox is a sexually transmitted disease, it is not conclusively proven. It looks like it, and we all think so, but we would need to culture the virus in semen to show that it is transmissible. It hasn’t been done so far.”
WHAT THE WHO SAYS
According to the World Health Organization, symptoms of monkeypox are usually fever, severe headache, muscle aches, back pain, low energy, swollen lymph nodes, and skin rashes or lesions. The rash usually begins on the first or third day of the onset of fever. The lesions may be flat or slightly raised, filled with clear or yellowish fluid, and then crust over, dry out, and fall off.
The number of injuries varies, from a few to several thousand. The rash usually appears on the face, the palms of the hands, and the soles of the feet. They can also appear in the mouth, genitals, and eyes.
In most cases, monkeypox symptoms go away on their own within a few weeks, but in three to six percent of reported cases in countries where it is endemic, it can lead to medical complications and even to death. Newborns, children, and people with weakened immune systems may be at risk for more severe symptoms and death from the disease.
The virus is spread through physical contact with someone who has symptoms. Rashes, body fluids (such as fluids, pus, or blood from skin lesions), and scabs are especially infectious. Ulcers, lesions, or sores can also be infectious, as the virus can be spread through saliva. Contact with objects that have been in contact with the infected person – such as clothing, bedding, towels – or with objects such as eating utensils can also represent a source of infection.
People who have the disease can be contagious while they have symptoms (usually in the first two to four weeks). “It is not clear whether asymptomatic people can transmit the disease,” according to the WHO. Today, anyone who comes into physical contact with someone with symptoms or with an infected animal is at greater risk of contagion. Those who live with infected people have a high risk of contagion. Health personnel, by the very nature of their work, are also at risk of exposure. You can reduce the risk of contagion by limiting contact with people who suspect they have the disease or who are confirmed cases.