The Chair of Infectious Diseases of the University of the Republic published an infographic on Monkeypox or mostly known as Monkeypox that as of May 25 there are 219 confirmed cases. It bears this name because the virus was first identified by Preben von Magnus in 1958 in laboratory monkeys (Macaca fascicularis).
Monkeypox is a viral zoonosis caused by an Orthopoxvirus, a genus of the Poxviridae family made up of double-stranded DNA viruses, which includes other viral species (smallpox virus and vaccinia virus) that affect mammals. The virus is mainly found in the tropical forest regions of Central and West Africa.
There are 2 viral strains classified according to their location.
Epidemiology
Non-zoonotic transmission:
- Direct physical contact, including sexual contact.
- Contact with belongings of other people who have injuries.
- Respiratory: through drops.
Zoonotic transmission:
- Handling or eating infected meat.
- Bites or scratches from infected animals.
- Contact with lesions or ears.
During infection, a generalized viremia occurs, so mother-fetus transmission is possible.
Pathogenesis and clinical manifestations
- Incubation period: 10 days on average (4-20 days)
- Prodromal or pre-eruptive phase: Fever 38.5 C, headache, cough, swollen lymph nodes, myalgia and malaise.
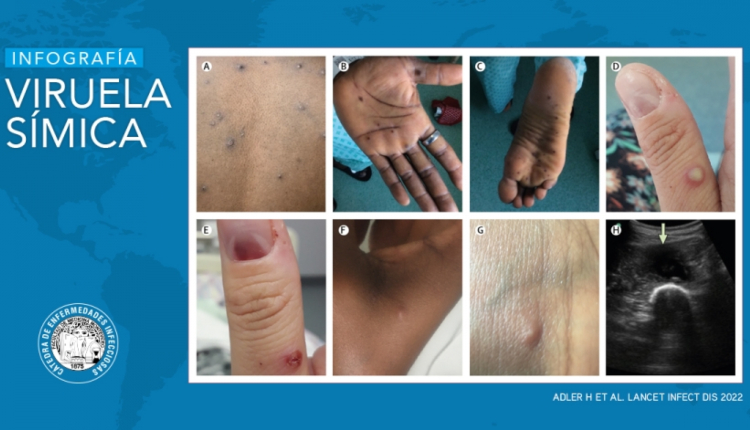
- Exanthematic phase (2-4 weeks): Rash in the form of blisters and scabs (Centrifugal rash, involving the face, palms, hands and feet). It is typical that ALL skin lesions are in the same evolutionary phase. Fever and swollen lymph nodes precede the rash by 24-72 hours.
Attributable mortality:
- 1-3% West African Strain
- 10% Central African Strain
Diagnosis
- Suspicious case definition: Vesicular rash with no explainable cause in any part of the body, 72 hours after presenting: fever (>38.5), associated with lymphadenopathy and myalgia/asthenia, in a patient from a non-endemic area in which Other common causes of rash have been ruled out according to the epidemiological context.
- Confirmed case: Confirmation by rt-PCR or DNA sequencing in a biological sample (lesion swab, scabs, vesicular fluids) of a suspected case.
Treatment
Monkeypox usually has a self-limited course, remitting in 2-4 weeks. However, in children and immunocompromised it can present complicated and life-threatening conditions.
There is no specific treatment to treat it, support measures (fever relief, analgesia and hydration) are sufficient in mild cases.
There are antivirals with in vitro studies such as tecovirimat, cidofovir and brincidofovir with little evidence. Its use is not widely available and is limited to strategic areas.
Prevention
- The period of greatest risk of transmission is the rash phase (with skin rashes).
- Health personnel must take respiratory and contact isolation measures in the event of a suspected and/or confirmed case.
- Isolation should be maintained until all lesions subside.
- Contacts of confirmed cases should be isolated for at least 21 days after contact, with monitoring of their symptoms.
- Family members and caregivers of confirmed cases should: a) avoid direct contact with the lesions, b) wear gloves and c) wash their hands properly, d) wear a surgical mask.
- There are 2 specific vaccines approved to prevent monkeypox, but availability is limited and they are not produced on a large scale:
- Jynneos: Inactivated virus vaccine.
- ACAM2000: Non-replicative attenuated virus vaccine.
- Smallpox vaccination administered until 1977 in Uruguay would confer a certain degree of cross-protection.